Southern California’s social care leaders gathered with a shared goal: to build a more connected, coordinated, and compassionate system of care. Healthcare providers, health plans, community-based organizations (CBOs), and regional collaboratives came together in Long Beach to explore how technology, partnerships, and community leadership can transform how people access support.
Throughout the day, one message rang clear: social care works best when it works together.
Read on for key takeaways:
Intentional partnerships allow healthcare and community partners to coordinate care and share information more effectively.
Investment in community partnerships is key, with health systems funding, training, and supporting CBOs to strengthen local networks.
New tools are enabling end-to-end social care, helping organizations meet state CalAIM requirements.
A special thank you to everyone who joined us and to our fantastic speakers for sharing their insight, experiences, and vision. The Summit reminded us that while policies and systems are complex, the mission is simple: connecting people to the help they need.
Highlights from the 2026 Southern California Social Care Summit
This year’s Summit featured 110 participants representing government agencies, healthcare providers, community organizations, and more:

Below are some of the key themes and takeaways from a day of learning and sharing.
Building toward end-to-end social care
Findhelp opened the Southern California Social Care Summit by sharing its vision for the social care continuum—and where the platform is headed next.
New capabilities, including post-acute care coordination and expanded behavioral health networks, are designed to support the full arc of a person’s journey, from identifying needs to delivering services and tracking outcomes.

“This is what we’re aiming for: end-to-end social care delivery.”
Andi Gillentine
VP of National Accounts, Findhelp
With programs like CalAIM reshaping California’s healthcare landscape, Findhelp is continuing to invest in tools that simplify reimbursement, automate workflows, and codify needs assessments using standardized clinical codes. These innovations help ensure providers and community partners can work more efficiently while meeting new requirements for closed-loop referrals.
Just as importantly, the platform is helping individuals navigate uncertainty—especially amid Medicaid redetermination challenges—by connecting them not only to healthcare services, but also to job opportunities, volunteer roles, and other pathways to stability.

From partnership to impact: Coalition networks in action
A panel featuring leaders from Inland Empire Health Plan, Inland SoCal United Way, and the Inland Empire Health Information Organization highlighted the power of regional coalitions like ConnectIE. Their shared goal was simple but ambitious: create a coordinated network where healthcare providers, social services, and community organizations could work from a shared understanding of each person’s needs.

“We’re connecting the healthcare side of things to the community side of things. A PCP [primary care provider] can see when 211 refers them to a food pantry or housing resource, for instance. Assessments are also a huge piece—providers not having to re-screen when it’s already been done that year.”
Rudy Valdez
Program Director, Inland Empire Health Information Organization
Coalitions enable organizations to securely share consented information, including referrals, assessments, and social risk factors. This longitudinal view helps reduce duplication and ensures individuals don’t have to repeat their stories every time they seek help.
But building trust took time.

“211 was worried we were coming into their space [as competitors]. We developed trust over two years through education and community training and now we have a strong partnership.”
Dr. Gabriel Uribe
Director of Health Equity Operations, Inland Empire Health Plan
Today, the Inland Empire coalition network supports thousands of individuals across Riverside and San Bernardino counties, improving coordination between health plans, 211 services, and CBOs.
Activating community networks through investment and engagement
Cedars-Sinai shared how they built their Community Connect Program, a Trusted Network designed to close social care gaps and strengthen partnerships with community organizations.
Before Findhelp, their approach was fragmented. Screening varied across teams, relationships with CBOs were siloed, and it was difficult to track outcomes. Creating a centralized network—and dedicating staff to maintain community partnerships—changed everything.

“We used to have inconsistent approaches to identifying SDoH needs, documenting them, and addressing them. Our community relationships were siloed, and it was difficult to identify trends. Providers had limited bandwidth and there wasn’t a team dedicated to closing social gaps. Then, we started working with Findhelp.”
Katie Hren
Director of Community Health Programs at Cedars-Sinai
In partnership with Findhelp, Cedars-Sinai established a multi-year grantmaking pilot that provided funding to CBOs addressing housing instability, substance use disorder, and mental health needs. The pilot ultimately helped secure a $400,000 annual budget to sustain and expand the work.
Cedars-Sinai leaders emphasized that building a strong network takes time; it took four to five years to gather enough data to make the case for sustained investment.

Turning technology into real-world impact
Health systems across Southern California are integrating social care more deeply into clinical workflows. UCI Health, which recently launched Findhelp across dozens of clinics, focused on ensuring staff and community partners were equipped to use the platform effectively.
Their approach prioritized quality over quantity—ensuring referrals were meaningful and partners were prepared to respond.

“You can pay for a platform, but it’s worthless if nobody is using it… The worst harm you can do to a community is to fund something short-term.”
Daniel Rivas
Director, Office of Community Outreach and Engagement at UCI Health
Children’s Hospital Los Angeles shared a similar philosophy, emphasizing the importance of regional collaboration to support youth health. Their Children’s Health and Wellness Collaborative brought together 16 organizations to align on shared goals and strengthen referral pathways.

“We know that youth health begins long before a child enters the hospital.”
Susan Gantan
Senior Program Manager at Children’s Hospital Los Angeles
Together, these efforts demonstrate how collaboration across healthcare and community sectors can address needs before they escalate into crises.
Connecting systems to power whole person care
As California continues implementing CalAIM (the state’s Medicaid 1115 Waiver demonstration), interoperability and data sharing are becoming essential. Leaders from Manifest MedEx explained how health information exchanges (HIEs) help bridge fragmented systems by aggregating clinical and social data.
By integrating Findhelp with HIE networks, providers will gain deeper visibility into referrals, assessments, and outcomes—allowing them to better coordinate care across organizations.
These integrations will help ensure that critical information follows individuals across healthcare and social care settings, reducing gaps and improving continuity.


“Before HIEs, data was very fragmented, across hospitals, labs, clinics, pharmacies, CBOs, counties, etc. Data was transferred via phone, fax, email. Through a sophisticated matching algorithm, HIEs determine whether someone is the same or a different person. We intake non-standard data and create a standardized output.”
Sara Fraley
Program Manager at Manifest MedEx
Designing with dignity in a changing policy landscape
With millions of Californians potentially at risk of losing Medi-Cal coverage, speakers emphasized the importance of proactive outreach and engagement. Community Care Hubs, like Partners in Care Foundation (a nonprofit in San Fernando Valley that integrates 100+ CBOs into a coordinated statewide network) are playing a critical role in coordinating services across hundreds of organizations.
Partners in Care’s key recommendations:
- Integrate Findhelp’s redetermination and community engagement tools
- Add redetermination dates to member information files (MIF)
- Leverage CBO + CalAIM networks and other allies
By integrating eligibility tracking, navigator workflows, and community networks, Findhelp is helping partners ensure individuals remain connected to essential benefits and services.

“Under H.R.1, up to 3.4 million members could lose MediCal coverage. The consequences are immediate and severe: rapid deterioration in health, avoidable ER [emergency room] use, and members returning to the system at higher acuity and higher cost. CBOs are ready to keep members connected, but this expanded role cannot be sustained without meaningful partnership and investment.”
June Simmons
President & CEO at Partners in Care Foundation
Powering a smarter, more connected safety net
The summit concluded with a look at Findhelp’s evolving platform, including new tools for ordering goods and services, coordinating post-acute care, and expanding behavioral health access. These innovations aim to create a more proactive and responsive safety net—one that connects people not just to referrals, but to real support and measurable outcomes.
We discussed how Findhelp, in partnership with California stakeholders, is supporting:
- Simplified referral workflows
- Connections between healthcare and social care providers
- Behavioral-health provider scheduling integration
- County-level coordination + technology infrastructure
“I really enjoyed connecting with so may inspiring people who are doing similar work in their hospitals and communities. I love how Findhelp encourages customers to share their experiences – there’s so much value in hearing the hands-on approaches, both big and small.”
A Population Health Coordinator who attended the Southern California Social Care Summit
Beyond the Summit: Our work in California
While the Summit provided a rich day of insight and connection, the real work continues — in homes, clinics, schools, and community hubs across California.
Some of the numbers that show the scale and momentum:
- 22,800 listed programs serving California
- 9.6 million users across the state
- 22 million searches for resources
- 220,000 social needs assessments completed
- 100% of counties have claimed programs
As of March 2026, we partner with more than 87 customers throughout the state to connect their patients, members, students, constituents, and clients to local resources. Our data and analytic tools can identify gaps in services and provide actionable insights to inform strategy and public policy.
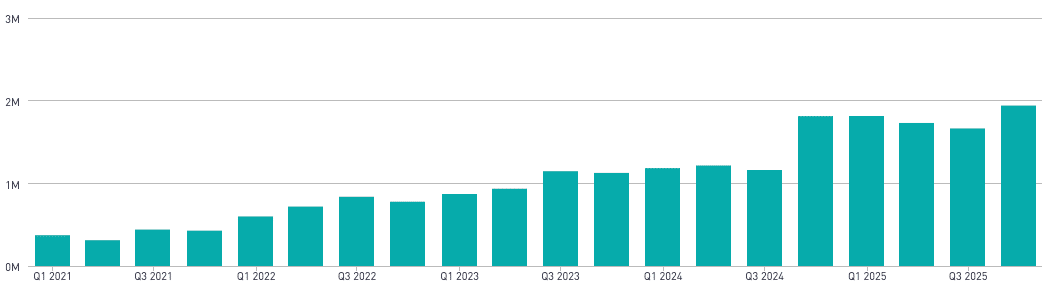
Together, with our California partners, we’re building toward a future where social care is not an afterthought — but a foundational part of how health, housing, and human services work together.
Let’s keep the conversation going
The Southern California Social Care Summit was a powerful reminder of what’s possible when purpose, people, and technology converge. If you’re interested in how Findhelp can support your work in California — whether you’re a health system, community-based organization, payer, or state agency — we’d love to chat.







