Operationalizing Community Engagement Requirements: Leveraging Integrations and Intelligence
In Part 1 of this series, “Medicaid 2027: Connecting the Ecosystem,” we discussed the need for a connected infrastructure to meet the upcoming Community Engagement requirements. In Part 2, we explore how Findhelp operationalizes that connection into a data-driven, intelligent workflow that enables states to access data that supports intelligent segmentation and ex-parte verification, while empowering Medicaid managed care organizations (MCOs), providers, and other stakeholders to support community engagement activities.

The federal government has established clear directives for states implementing Medicaid community engagement requirements: states must prioritize ex parte verification, using available data to verify eligibility without beneficiary action.
In this post, you’ll learn:
How Findhelp connects states, plans, providers, CBOs, & beneficiary for intelligent segmentation.
How guided compliance pathways, with smart logic and configurable exemptions, can replace complex paperwork.
How to enable your members and navigators to quickly and easily complete applications.
To meet the Federal standard, many states are working to connect their internal systems, which can be a heavy lift for those without a unified eligibility and enrollment process. However, internal data alone can be insufficient to build a complete picture of a member’s status. Without connecting to external ecosystems, states are left with a larger, unsegmented population to manage manually. Furthermore, unless eligibility data is shared with partners, MCOs and healthcare providers are unable to effectively support this large-scale effort.
This is where Findhelp bridges the gap. Through our community engagement workflow, we ingest, aggregate, and share this critical eligibility data.
Here is how our infrastructure manages an intelligent workflow for States, MCOs and provider organizations.
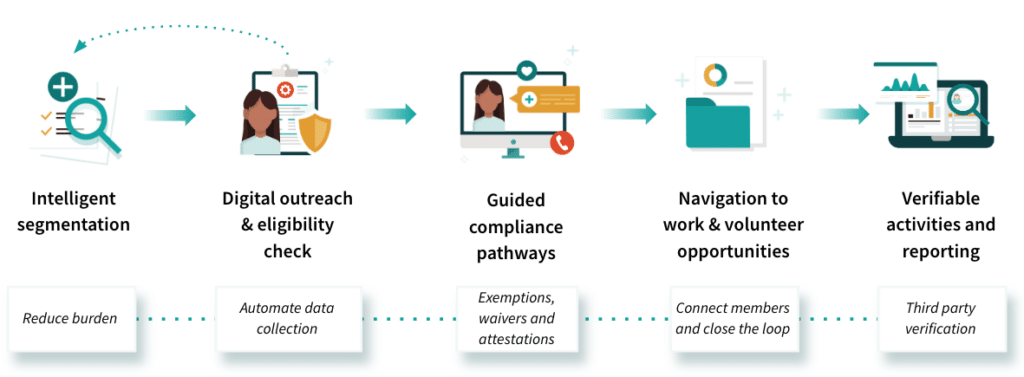
Ingesting data for intelligent segmentation
The foundation of the workflow is the ability to segment members based on their real-time status. Findhelp handles this by acting as the connectivity layer between the State’s system of record and the community partners who need visibility.
- Flexible Integration: Findhelp connects to the State’s eligibility and enrollment system via real-time API or by ingesting batch files containing key data points, such as Eligibility Status, Redetermination Date, and Ex Parte flags.
- The Unified Member Profile: We surface this data directly in the member’s profile. When an MCO or Navigator performs a member lookup, they can see a real-time view of the member’s engagement status. MCOs can instantly identify members who require intervention, ensuring resources are focused on those who need them.

Guided eligibility check (eCheck) and compliance pathways
For members needing assistance, Findhelp replaces complex paperwork with a guided compliance pathway that gathers data that might not be available to the state in their existing systems. This can include a recent medical encounter, diagnosis or temporary hardship. Findhelp’s eCheck, a configurable, logic-driven workflow, identifies these data points to further segment members.
- Configurable Exemptions: Our environment is fully configurable to match your State’s specific policy landscape. Whether you have adopted optional temporary exemptions or specific hardship criteria, the workflow adapts to capture them.
- Smart Logic: The interface uses plain-language questions to identify “invisible” exemptions, such as recent medical events that haven’t hit the claims file yet, changes in caregiving status, or undiagnosed conditions.
- Streamlined Proof: If a member claims an exemption, they can snap a photo of a supporting document (like a doctor’s note or school schedule) and upload it instantly to our secure platform.
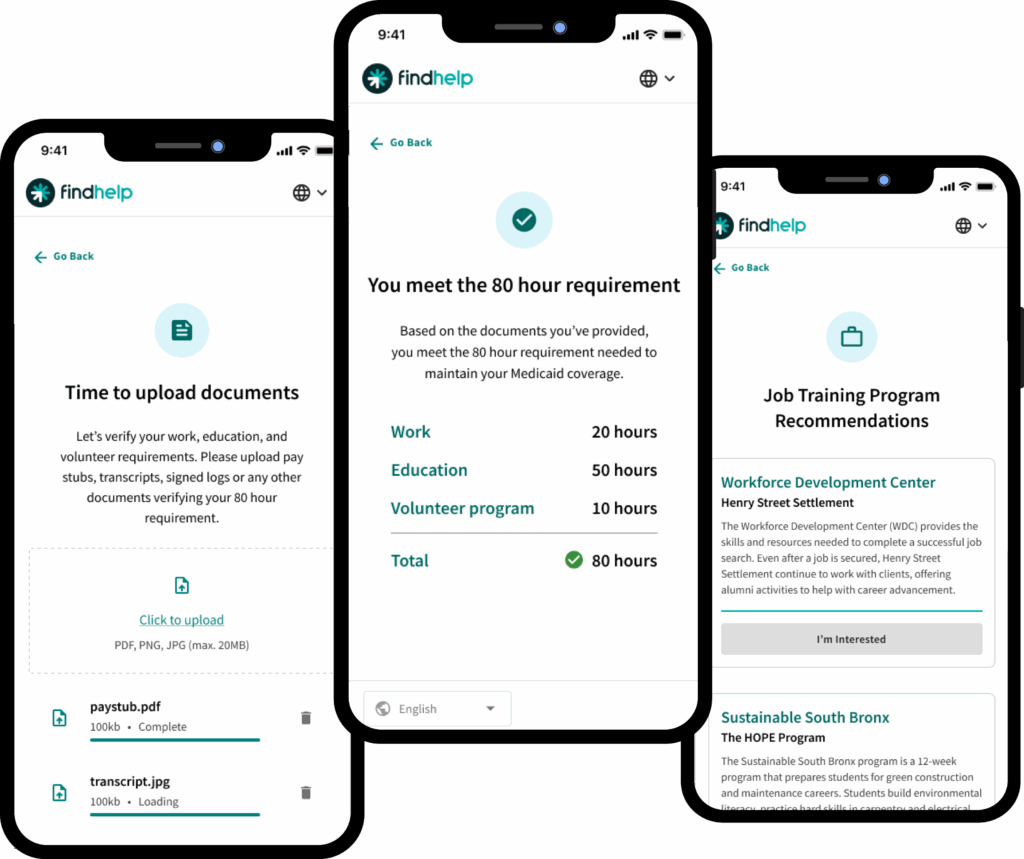
Once collected, we package this information and transmit it back to the State or enable the member to submit it directly. This transmission workflow is fully configurable, ensuring the data arrives exactly how and when the State’s system requires.
Navigation and verifiable activities
For members who must complete additional community engagement hours and report them, Findhelp leverages our nationwide network to shift from simple navigation to verifiable activities.
- Search & Connect: Members access our curated network of workforce, education, and volunteer programs.
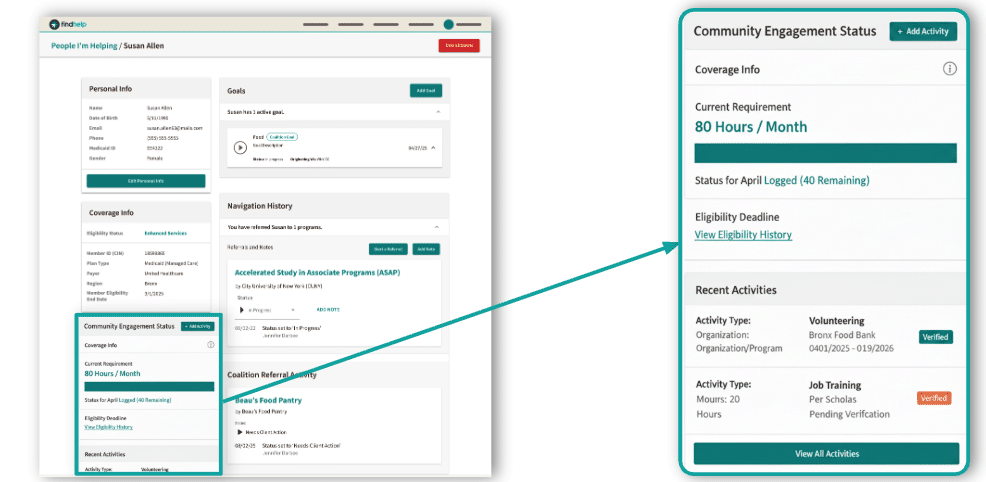
- Closing the Loop: When a member selects a program, Findhelp generates a digital referral. Community partners can confirm the member’s participation. Referrals and completed hours are tracked in both a member and navigator view.
- The Verified Record: This “closed loop” creates a third-party verified data point that is reportable to the state, replacing self-attestation with audit-ready proof.
- Addressing Barriers to Work: Our platform allows members to search for and connect with essential support services, like childcare, transportation assistance, and work clothing, removing the barriers that make employment and community engagement difficult to maintain.
This workflow is designed for both self-service (members searching on their own) and assisted navigation (Navigators and Case Managers helping members connect to resources).
A unified path forward
Operationalizing the 2027 requirements offers a unique opportunity to unify the Medicaid ecosystem.
By leveraging Findhelp to ingest external data and share intelligence, States gain a scalable force multiplier—effectively expanding their efforts through MCOs and community partners. This proactive visibility allows stakeholders to intervene in a timely manner, supporting Medicaid members in community engagement activities and pathways to economic mobility.
What’s next?
Now that we have defined the workflow, how do we build the infrastructure?
In Part 3, we’ll look at Deployment Models, and in Part 4, we’ll break down the Data Model that powers these integrations.








